Opening eyes to chronic pain’s grip on the psyche
Jennifer De La Rosa, PhD, draws on life experiences and scientific expertise to study chronic pain and its relationship with mental health.

Jennifer De La Rosa, PhD, uses lived experience to inform her chronic pain research. While in high school, she created this piece of art to illustrate her experience with migraine headaches.
Illustration courtesy of Jennifer De La Rosa, PhD
When Jennifer De La Rosa, PhD, first encountered the havoc that chronic pain could wreak on a life, the experience was harsh and personal.

Jennifer De La Rosa, PhD, is an assistant research professor in the Department of Family and Community Medicine at the University of Arizona College of Medicine – Tucson and strategy director at the U of A Health Sciences Comprehensive Center for Pain & Addiction.
Photo by Kris Hanning, U of A Health Sciences Office of Communications
De La Rosa, who is the strategy director for the University of Arizona Health Sciences Comprehensive Center for Pain & Addiction, remembers watching her grandmother, Christine Wise, struggle with rheumatoid arthritis and severe clinical depression. She recalls the image of a woman tormented by angst, frustration and despair. Wise’s health issues forced her daughter – De La Rosa’s mother, Sally Schultz, PhD, – to grow up quickly. While in grade school, Schultz took on a caretaker role for her mother.
The experience helped Schultz, and then De La Rosa, define their career paths. Schultz became an occupational therapist and clinical faculty member with a focus on psychosocial rehabilitation. Like her mother, De La Rosa pursued a career in higher education.
De La Rosa said her mother and grandmother, as well as trials in her own life, taught her how important it is to empathize with the people behind the research statistics.
“My mom always emphasized the need to connect with people on what motivates them, not what motivates you, in promoting adaptive rehabilitation,” said De La Rosa, who is an assistant research professor in the Department of Family and Community Medicine at the U of A College of Medicine – Tucson. “For instance, a clinician might want to coax a child to play a game or an adult to do a task that could help them. My mom is very good at using what motivates somebody to promote their engagement in care, and that’s something I really value and try to bring forward in my work as well. It’s not about me and what I want. It’s about the person, and what they really want.”
Helping people thrive
De La Rosa found her professional calling at the Comprehensive Center for Pain & Addiction, where she works with a team of experts devoted to reimagining and transforming health care for pain and addiction.
“Dr. De La Rosa truly advances science with a creative mind,” said professor Beth Meyerson, PhD, one of De La Rosa’s mentors, policy director of the Comprehensive Center for Pain & Addiction, and director of the Harm Reduction Research Lab in the Department of Family and Community Medicine. “She is brilliant and willing to suspend disbelief to propose the unconventional for the improvement of health.”
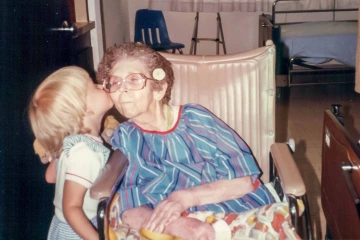
De La Rosa, left, shares a tender moment with her grandmother, Christine Wise, in 1986 in Amarillo, Texas.
Photo courtesy of Jennifer De La Rosa, PhD
De La Rosa leads several projects including PeerWORKS, a paraprofessional training program that helps individuals with substance use disorder experience become certified peer support specialists to help others. Her research focuses on the intersection of chronic pain and mental health. Her two most recent papers, both published in the journal PAIN, shed light on the prevalence of mental health issues that co-exist with chronic pain.
One study found that 1 in 20 adults in the U.S. experience the co-occurrence of chronic pain and anxiety and depression, which can result in functional limitations in daily life. A follow-up paper showed that adults with chronic pain are more likely to experience symptoms of anxiety and depression than those without chronic pain, yet they access mental health care at lower rates and are less likely to have their mental health needs met in treatment.
The findings put a spotlight on hidden troubles experienced by people who live with chronic pain.
“Dr. De La Rosa’s research into the relationship of chronic pain and mental health issues uncovered a great need in our society that, when addressed, will improve the lives of millions of people,” said Todd Vanderah, PhD, director of the Comprehensive Center for Pain & Addiction, Regents Professor and head of the Department of Pharmacology at the College of Medicine – Tucson, and one of De La Rosa’s mentors. “Jennifer is incredibly intelligent and passionate about helping those that suffer from chronic pain and mental health. One of the things I value most about Dr. De La Rosa is that she truly cares about her work and the people who will ultimately benefit.”
Pain is personal
De La Rosa’s mother and grandmother taught her much about living with chronic pain, but the harshest teacher was her own experience. As a child and young adult, De La Rosa dealt with frequent migraine headaches bad enough to cause her to vomit and retreat to a dark room. She still gets migraines occasionally but they are less disabling now, and she has personalized her own approach to managing the pain.

(From left) De La Rosa watched Schultz receive her doctorate in 1991 at the University of North Texas, and Schultz watched her daughter receive her doctorate in 2013 at the University of Arizona.
Photo courtesy of Jennifer De La Rosa, PhD
“People really do have a lot of experiences with pain over a lifetime – not just one pain experience usually, but several, like a string of pearls,” she said. “We take these experiences: our response to them, and what they mean to us, into every area of our lives.”
De La Rosa’s experiences led to a professional passion and drive to combine sociology and data science in research that will improve the lives of people who live with chronic pain.
“I’m using a lot of secondary data analyses to understand the dynamics of chronic pain and mental health. Moving forward, I intend to work on real-world applications,” De La Rosa said. “How can we develop empowerment and functional resilience in a person? How can we prevent somebody’s pain from becoming extremely limiting, not only in terms of their function, but also in them being able to live the life they want to live?”
De La Rosa enjoys speaking to people about the ways pain affects them and their loved ones. She says chronic pain and mental illness often feed off one another. In her grandmother, pain limited her mobility and independence, exacerbating her depression.
But there is hope, De La Rosa says, in the darkness. The ability to take ownership over one’s experience can help someone adapt to or even begin to improve their current situation, reducing their experience of pain.
“I was raised with this real concern for the needs and experiences of those with chronic pain, as well as the importance of hope,” De La Rosa said. “My mom taught me it is important to design interventions in a person-centered way, selecting purposeful activities and goals that people consider meaningful. Experiences of meaning and mastery promote hope, adaptation and recovery.
“I think there is a certain humanity that we can introduce into research when we acknowledge that we are all people with multitudes of experiences in our histories, many of which include pain or struggles with mental health.”
Experts
Jennifer S. De La Rosa, PhD
Assistant Research Professor, Department of Family and Community Medicine, College of Medicine – Tucson
Strategy Director, Comprehensive Center for Pain & Addiction, U of A Health Sciences
Todd Vanderah, PhD
Regents Professor and Head, Department of Pharmacology, College of Medicine – Tucson
Director, Comprehensive Center for Pain & Addiction, U of A Health Sciences
Professor, Department of Anesthesiology, College of Medicine – Tucson
Professor, Department of Neurology, College of Medicine – Tucson
Co-Director, MD/PhD Program, College of Medicine – Tucson
Member, BIO5 Institute
Beth Meyerson, PhD
Professor, Department of Family and Community Medicine, College of Medicine – Tucson
Policy Director, Comprehensive Center for Pain & Addiction, U of A Health Sciences
Director, Harm Reduction Research Lab, Department of Family and Community Medicine, College of Medicine – Tucson
Contact
Phil Villarreal
U of A Health Sciences Office of Communications
520-403-1986, pvillarreal@arizona.edu

